Healing Hearts in Honduras
A Duke team brings hope and heart valves to patients running out of time
Imagine a doctor saying you need surgery to replace a heart valve, and if you don’t get it you will die from heart failure within two years.
If you live in Honduras, once you get that diagnosis at a public hospital, the doctor will hand you a list of the items needed for the surgery: saline solution, sutures, gloves, an oxygenator, pain medication, and a heart valve. As the patient, it’s your responsibility to find— and buy —the items on that list. The cost of a mechanical heart valve alone is $4,000 to $7,000. The average Honduran’s salary is $600 a year. The country is one of the poorest in the Americas.
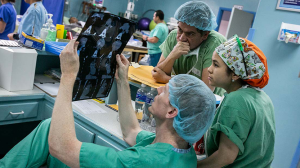
In July 2019, a team from the Duke University Health System and Duke University School of Medicine flew from Durham to the capital city of Tegucigalpa, Honduras, to perform heart surgeries at Instituto National Cardiopulmonar (INCP). The surgeries prolonged the lives of 11 patients who did not have the means to pay for heart valve surgery.
The team of 18 from Duke included cardiothoracic surgeons, physician assistants, surgical residents, perfusionists, a biomedical engineer, intensive care nurses, operating room nurses, thoracic surgery residents, cardiac anesthesiologists/intensivists, and a Duke University School of Medicine student.
The monumental effort to coordinate the personnel, medicine, equipment, approvals, and funding began more than a year before the trip when Honduran native Alejandro Murillo Berlioz, MD, was interviewing for a position as a resident at Duke. During his interview Murillo was asked to describe his medical career goals. His answer was succinct: “I’m a Honduran. I was born and raised there. So my goal is to get the best training there is, but then become an agent of change in my country for my people.”
A few months later, Murillo matched with Duke and started his residency with the Integrated Thoracic Surgery Residency Program. Shortly after arriving in Durham, he received an email from Carmelo A. Milano, MD, Duke heart and heart transplant surgeon, chief of the Section of Adult Cardiac Surgery, surgical director for the Left Ventricular Assist Device (LVAD) Program, and professor of surgery. Milano welcomed Murillo to Duke and wrote, “You spoke about wanting to help Honduras. Let’s talk more about it.”
Twelve months later, the Duke team landed in Tegucigalpa ready to help patients and, more importantly, train Honduran surgeons and nurses how to best replace heart valves and care for recovering patients in a country where more than half the population lives in poverty.
“AN AMAZING EXPERIENCE”
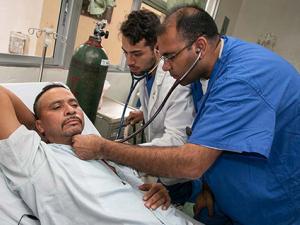
Second-year medical student Fabian Jimenez Contreras, BS’18, jumped at the chance to travel with the team to Honduras. His travel was funded by a grant from the Charles T. Watt, MD, Travel Fellowship. Jimenez, who speaks Spanish fluently, was able to have lengthy pre-operative conversations with the patients. Jimenez determined what kind of family support the patients had and what their home lives were like. He discussed with them the choices of a mechanical heart versus a bioprosthetic, and talked about the risks involved in the surgery. Jimenez would end the conversations discussing each patient’s post-op medications and follow-up care.
“One reason this experience was so valuable to me is because it gave me a little window into working as a team,”” Jimenez says. “My second year of medical school is going to be all about working in a team environment.”
The trip was eye opening, he says. “I will take the experience with me forever. It will help me immensely in my future training, and one day as a heart surgeon,” says Jimenez. “I don’t think I’ll ever forget the kind of work that we were able to do with limited resources. There are people out there that really need our help, and we can’t forget about them. The patients are such wonderful people. The patients were humble and extremely grateful to get the surgery. Many of them commented how we were saving their life. It was truly an amazing experience that I will take with me throughout my medical training.”
STREP AND RHEUMATIC HEART DISEASE
In many countries without developed heath care systems, streptococcal infections are not treated with antibiotics the way they would be for a child or young adult patient in the United States. If a strep infection is not treated, it can lead to rheumatic fever. In turn, rheumatic fever becomes rheumatic heart disease when antibodies working against the disease begin to “attack” the heart valves. Over months or years, the valves become hardened and do not function properly. Patients show symptoms of shortness of breath when the valves are compromised. As the disease progresses, the patient will experience shortness of breath even when doing simple tasks like tying their shoes.
Heart valve replacement surgery removes the diseased valve and replaces it with a mechanical or bioprosthetic valve. The surgeons recommend the kind of valve based on the age of the patient and other factors.
According to one of the lead heart surgeons on the Duke team, Adam R. Williams, MD, assistant professor in the Division of Cardiothoracic Surgery, once a patient becomes symptomatic he or she will need a replacement valve within two years or face the risk of premature death.
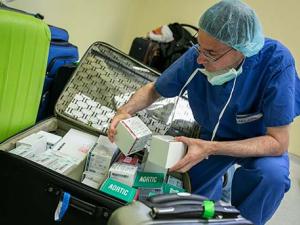
For the trip to Honduras, the Duke team took a number of valves and pacemakers donated by manufacturers in the United States. The valves were packed in carry-on bags while other equipment—including a heart-lung machine—was sent ahead to Honduras earlier.
Once the team finished the surgeries in Honduras, medical equipment was left at the hospital. Hugo Orellana, MD, the chief of cardiothoracic and vascular surgery at Hospital Escuela, which includes the INCP, reported he now has 67 valves, along with annuloplasty rings, pacemakers, bicameral pacing boxes, and an upgraded heart-lung machine—all equipment he didn’t have before the Duke team arrived. The hospital in Tegucigalpa has a waiting list of over 100 patients who need valve replacements.
“We have improved Dr. Orellana’s knowledge and comfort with the procedure,” says Milano. “He’s just limited to how many replacements he does based on limited resources.”
A LONG-TERM RELATIONSHIP
Team leaders hope the July trip was just the beginning.
“I hope this becomes a long-term relationship between Duke University and Honduras, where we can continue to provide valve replacements for patients who otherwise would never have surgery,” says Williams.
Murillo is planning to use a research gap year to return to Honduras for six to eight months and develop a heart valve replacement program. He hopes he can arrange for a Duke team to visit Honduras twice a year, to do valve replacements and train Honduran surgeons.
“My dream would be for this to be a program by the time I finish training,” Murillo says. “So we’re talking about seven to eight years for it to be a program. If that happens, I can come to Honduras and do everything I’m trained to do. It would be a dream to come to Honduras and run it and help all these people.”
Dr. Jatin Anand, MD, a resident in cardiac surgery, says Murillo’s support will help establish a long-term collaboration between Duke and the Honduran hospital.
Anand adds that for the trip in July, “We have lots and lots of people,” who did not go to Honduras, “to thank for making the trip possible and for making it go as smoothly as it did.” People from a number of areas at Duke University Health System, Duke University School of Medicine, and the Private Diagnostic Clinic (PDC) supported the trip.
“TRANQUILO”
Although there were a few Spanish speakers on the team, some needed assistance communicating with the hospital staff, patients, and doctors.
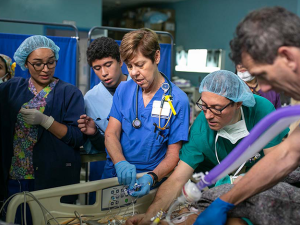
“The Duke intensivist talked to us about helping the [Honduran] nurses learn how to more rapidly progress patients,” says senior ICU nurse Myra Ellis, MSN, RN, CCRN-CSC, who has worked at Duke for 25 years. “I would talk to the translator and tell them, ‘When the patient wakes up, they just need to know that they have to wake up and take deep breaths. We just have to coach them to be calm.’”
Ellis doesn’t speak the language. “But I did learn a great Spanish word, which was ‘tranquilo,’” she says. “It means tranquil or calm. It doesn’t even need translation.”
Neither did the gratitude the patients and their loved ones expressed to the team members and their Honduran colleagues.
“The patients would just thank everybody. The families did more of that. They were incredibly grateful,” says Ellis.
The trip did more than just save 11 patients. The object was to jump-start a cardiac care program that the Honduran teams will continue as they work to help more people in need.
“We shared a lot of our perioperative care that we do here at Duke with the local team there,” says Williams. “The goal was not just come down there and do surgery, but to create an environment where they can continue doing surgery in Honduras and continue caring for these patients.”
The Duke team got a lot out of it too.“It was very exciting for the entire team to be able to go down and do something like this,” says Williams. “Going into the operations was exciting, and fortunately our surgeries went well and the patients feel better. At the end of the week, it was probably the most gratifying professional experience I’ve ever had.”
Duke University Medical Center and the Duke Heart Center were the primary funding sources for the mission trip with Tom Owens, MD, Joseph Rogers, MD, and Jill Engel, DNP, serving as important administrators of the grant.
Sponsors included: Abbott; American School of Tegucigalpa; CryoLife; Honduran Ministry of Health; Honduras at Instituto National Cardiopulmonar, house staff ; Lady Lee Corporation; Medtronic; U.S. Army Bravo Medical Element – Honduras.